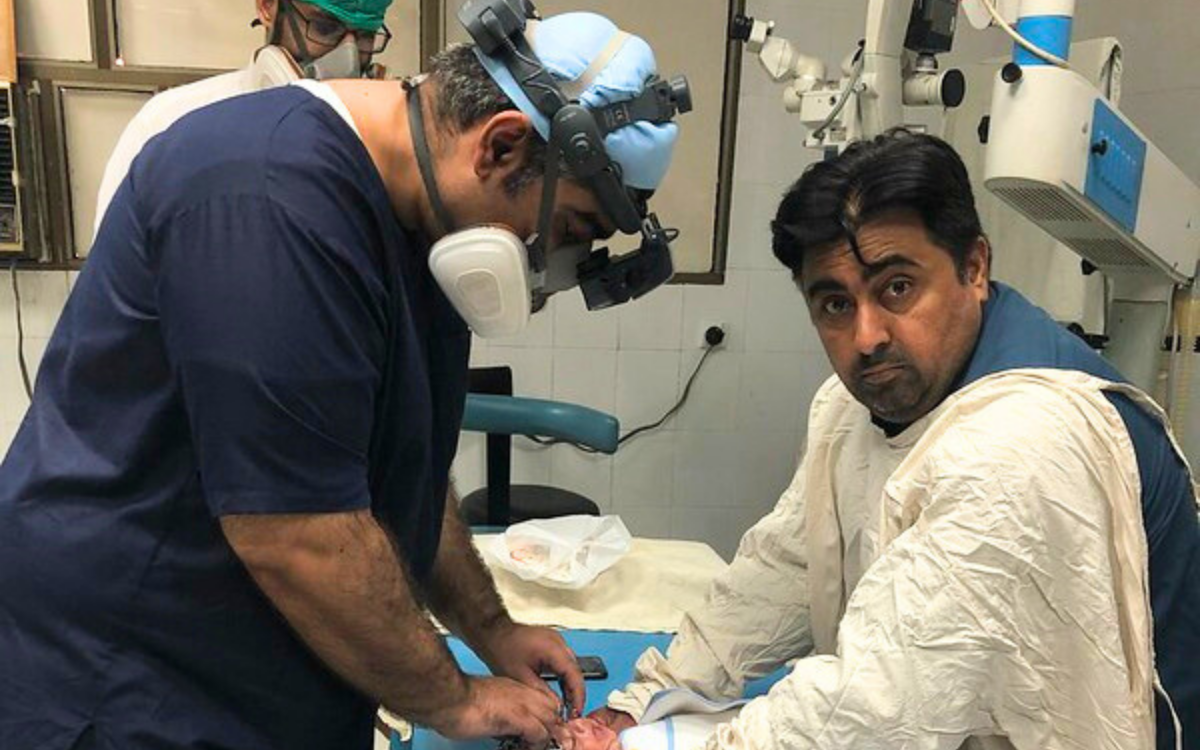
Screening for Retinopathy of Prematurity done at Eye Department MTI Khyber Teaching Hospital, Peshawar, Pakistan. Photograph: Sadia Sethi
A new prospective study conducted at a major public hospital in Pakistan reveals a significant rate of severe retinopathy of prematurity (ROP) among preterm infants and underscores the substantial clinical and service burden associated with ROP screening in resource-limited settings. The findings, published in BMC Ophthalmology and including researchers from the International Centre of Eye Health, offer critical insights for neonatal eye care planning in similar contexts.
Retinopathy of prematurity is a potentially blinding eye condition that affects premature infants with low birth weights and early gestational ages. Timely screening and treatment can prevent lifelong vision loss, but delivering these services requires sustained clinical capacity and careful coordination, especially where health systems are already stretched.
In this study at Lahore General Hospital, researchers followed all preterm infants eligible for ROP screening between 2015 and 2021 — defined as those born at ≤ 35 weeks gestational age or weighing ≤ 2000 g at birth. Examinations were carried out by experienced ophthalmologists according to established screening criteria, and infants were tracked through the diagnostic process to identify severe disease.
The study found that the rate of severe ROP requiring treatment was notable, reflecting both the underlying risk in this high-vulnerability population and the ongoing need for systematic screening services. The authors highlight that a substantial proportion of screened infants met criteria for clinically significant disease — indicating a heavy clinical workload for neonatal units and ophthalmology services in tertiary hospitals.
Importantly, the researchers also assessed the operational burden of maintaining a screening programme over multiple years. From 2015 to 2021, ROP screening contributed a considerable share of workload for ophthalmologists and neonatal teams, with follow-up examinations and treatment planning adding layers of complexity to routine clinical care. The authors emphasise that screening protocols, referral systems, and integration with neonatal care are essential to meet both demand and quality standards.
These results have implications for policy and programme planning in Pakistan and other low- and middle-income countries where ROP prevalence is rising with improved survival of preterm infants. They highlight the need for health system strengthening, including training of additional personnel, equipment investment, and inclusion of ROP screening in broader neonatal care strategies.
The study’s authors recommend that policymakers and health planners use this evidence to support targeted investments in ROP services, with an emphasis on sustainable screening pathways that can be scaled beyond tertiary hospitals to regional and district levels — potentially reducing preventable childhood blindness from ROP across larger populations.
Publications
Moin M, Mian LS, Martinez-Hussain M et al. Severe ROP rate and assessment of the burden of ROP screening at a single tertiary care public hospital in Pakistan. BMC Ophthalmology. October 2025. https://pubmed.ncbi.nlm.nih.gov/41131487/