A team led by the International Centre for Eye Health (ICEH) have demonstrated a new indicator that assesses how long people at risk of cataract need to travel to treatment.
Increasing age is a risk factor for developing cataract. Therefore, when planning services for age-related cataract, the group of interest tends to be people 50 and over. Evidence has also shown that older people living in rural and remote areas globally are more likely to develop sight loss from the condition as they are less able to access services.
Previously, ratios of the number of cataract surgeons and facilities that provide cataract surgery to the number of people in the population have been used, alongside other indicators, to demonstrate the access that people in that population have to treatment.
However, the travel time to treatment is also of importance. Service providers may be available and ready, but if they are not distributed among communities in such a way that all people can access them, they may not be used by certain groups.
New research by ICEH has demonstrated for the first time an indicator that countries can use to understand how many people aged 50 years and older live within a given travel time (e.g. 1 hour or 2 hours) of a public health facility providing permanent cataract surgical services.
To demonstrate the indicator, the researchers looked at data from Kenya, Malawi and Rwanda. They started by looking at publicly available lists of health facilities, then asked a ‘key informant’ in the eye care field from each country to assess which centres provided permanent cataract services.
For each country, both the number of people 50 years and older per location and the travel time across each area was estimated. Travel time was from a ‘friction surface’ map, which breaks down the world into 1km2 pixels and estimates how long it takes to get between them, dependent on the quality of roads, transport and terrain.
To this map of population and travel time for each country, the location of cataract surgical facilities were then added. Travel time was then assigned to levels: either 1 hour or less, 1-2 hours, 2-3 and more than 3 hours travel time to the nearest facility.
The number of permanent cataract facilities for each country, and the population aged 50 years and older able to reach them within in one or two hours were:
| Country | Population over 50 able to reach a permanent facility in ≤1 hour | Population over 50 able to reach a permanent facility ≤2 hour |
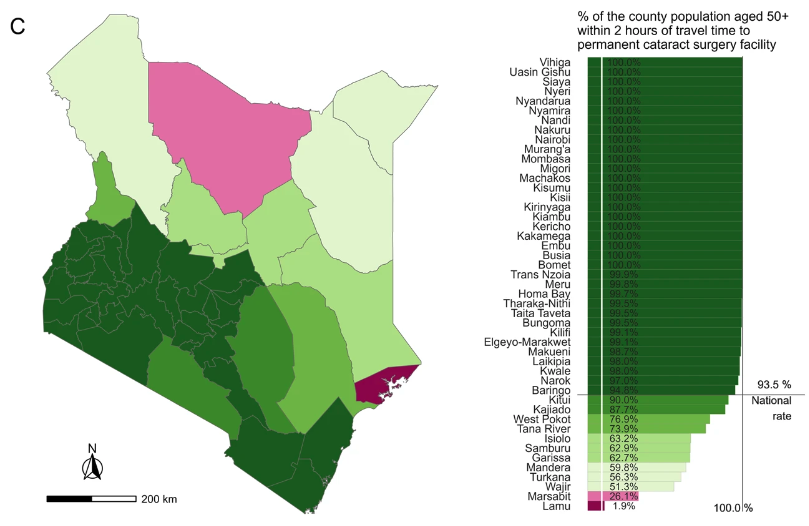
| Kenya | 84.1% | 93.5% |
| Malawi | 52.2% | 92% |
| Rwanda | 77.5% | 97.2% |
Full maps and travel times per region of each country are available in the publication here.
Only a small percentage of people in all three countries lived more than 2 hours from a facility, with some intriguing outliers. For example, in Malawi, everyone aged 50 years or older in the northernmost two counties lived further than two hours travel time to a permanent facility.
This indicator also flagged up some potentially important new findings for planning services. In Rwanda, when looking at the number of cataract facilities per 100,000 population it was higher in one province than another. Yet, when using the travel time indicator, the reverse was true. Despite having more facilities, fewer people were able to access them within a defined journey time.
The work provides an exciting new addition to measures of eye health access used for service planning. Used alongside other indicators, such as effective cataract surgical coverage and cataract surgical rate, it can help to identify those most at risk of living with sight loss due to cataract.
The authors note a few limitations of the new indicator. Improvements in the data inputs, finer detailed friction surfaces and locally validated travel times would likely improve the readings. Future research will aim to strengthen a standardised methodology for the indicator, allowing its use alongside other more established ones.
Publication
McCormick, I., Nesemann, J.M., Zhao, J. et al. Travel time to cataract surgical services in Kenya, Malawi and Rwanda: demonstrating a standardised indicator of physical access to cataract surgery. Eye (2023). https://doi.org/10.1038/s41433-023-02790-8